Artificial Intelligence and Ultrasound: Preparing for the Future of Medicine
- Nov 28, 2023
- 5 min read
AI is an umbrella term which includes the theory and development of computer systems to perform tasks normally requiring human intelligence such as speech recognition, visual perception, decision-making and prediction (Hardy & Harvey, 2019). AI technology is fast becoming the future of medicine with increased uptake in users and applications. It is adept at streamlining processes and standardizing images. It also shows merit in the detection and classification of neoplasms. Medical staff believe that AI will be incorporated into medical practice within the next 5-10 years (Swar et al., 2018). Sonographers and radiologists have always been closely interwoven with technological advancements and so the integration of AI is inevitable. However, AI will bring with it a decisive shift in the role of digital imaging operators and radiologists.
Deep Learning
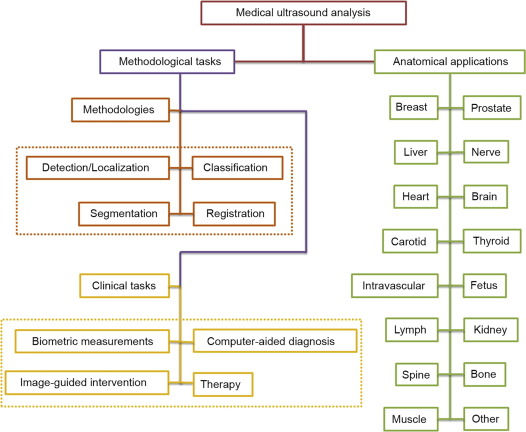
Deep Learning is a branch of machine learning which can perform mid-, and high-level image analysis, including lesion/nodule classification, organ segmentation, and object detection. DL can also be applied to biometric measurements, quality assessment, and interventional procedures (Liu et al., 2019). DL is currently being applied to breast, prostate, liver, cardiac, thyroid, fetal, lymphatic, spinal, and intravascular digital imaging review systems across the DI spectrum. It is also very applicable in 3D Volume rendering, whereby traditional 2D images are converted mentally by the operator and radiologist to obtain results, and assumes volumetric measuring of ellipsoidal masses, which causes discrepancy and error in classification, biometric volume rendering and extension of pathology. DL can be applied to these 2D images and render a more accurate 3D volume representation of sonographic findings (Liu et al., 2019).

Clinical Setting and Patient Experience
Even before a patient arrives for their procedure, AI is able to improve patient experience and outcome. AI can be used to vet exams, by checking clinical indications and patient identifiers against imaging modalities and techniques to improve efficiency and enhancing cost-savings measures by confirming imaging exams and rejecting invalid requisitions (Hardy & Harvey, 2019). It has powerful data analysis capabilities which allow it to obtain, sort through, and process an entire catalogue of historical patient-related data to ensure proper examination, medical history, and compliance (Habuza, et al., 2021). This reduces scheduling errors and streamlines patient time in clinic or hospital settings, which also allows for increased work volume within digital imaging departments (Habuza, et al., 2021).
Once within the department, the applications of AI are limitless, but for the sake of this post we will be focusing on diagnostic medical sonography. That being said, AI systems can be used to assess patient positioning for CT and MRI imaging, reducing exposure times and optimizing contrast volumes and injection rates (Hardy & Harvey, 2019).
Diagnostic Medical Sonography
Diagnostic medical sonography (DMS) is one of the most used and growing digital imaging tools since it is cost-effective, has no radiation, and is non-invasive. However, it remains subject to user variability and diagnostician experience levels (Liu et al., 2019). AI is being developed for tumour detection, biometry, and reporting for thyroid, breast, liver, and fetal sonograms (Liu et al., 2019). AI has been shown to be more accurate in the detection, documentation, and characterization of neoplasms, often reducing the need for invasive fine needle aspirations (Liu et al., 2019).
DMS is the gold standard imaging modality for prenatal imaging and is already well-adapted to AI. Sonographers already use AI for fetal biometry, which excels at interpreting shapes beyond the elliptical presumption of automated calibration tools (Looney, et al., 2018). AI is also proving particularly powerful for placental health. Placental volume is linked to birth weight and is used to determine the health outcomes of fetuses. Unfortunately, organ volume sampling is inconsistently applied due to technical constraints, user discrepancy, and being time-consuming in nature. AI can be used to quickly and accurately obtain 3D volume rendering of ultrasound images of first-trimester placentas better to predict preeclampsia and fetal growth restriction (Looney et al., 2018). There remains a tendency for AI models to overestimate placental size, and computer models have difficulty distinguishing between myometrial and placental tissue (Looney et al, 2018). With improvements in AI technology, this appears to be a promising future application for DMS and AI integration.
AI can further improve the speed and efficiency of reporting through automatically generated reports, data transfer, and QA auditing. This can also standardize how exams are reported, highlighting key findings and improving acting physician communication practices (Hardy & Harvey, 2019).
Pitfalls

Increasing automation of tasks for radiographers can increase patient volume, thus decreasing wait times. However, mounting evidence shows that this increased burden can negatively impact morale, role satisfaction, and burnout (Hardy & Harvey, 2019). Adaptations to the roles and responsibilities of radiographers and radiologists will be vital in adopting AI technology in digital imaging. This may include cross-training, expanding the responsibilities, or redirecting staff roles within or beyond direct patient interaction.
AI can have a high error count, up to 87%, depending on application, model, and user, so training, IT costs, and ongoing quality assurance evaluation methods are critical (Botwe, et al., 2021; Lundstrom & Lindvall, 2023). Other limiting factors to AI uptake include the upfront cost of technology, fear of cyber vulnerability, insufficient staff training, and fear of job insecurity (Botwe, et al., 2021). Studies show that proper engagement, training, integration, and adaptation of radiographers in their role reflect positive attitudes towards AI, and this study shows that 80.8% of participants believe AI is the future of diagnostic imaging (Botwe, et al., 2021). Interestingly, this statistic was consistent across all demographics such as age, gender, race, education level, and employment (Swar et al., 2019).
Finally, while AI was initially promoted as an equalizer tool, excellent at promoting fairness by eliminating user bias, studies suggest that AI can actually enhance biases as it is integrated into the computer model system (Lundstrom & Lindvall, 2023). This is further supported by AI training statistics, which reflect a narrow population spectrum (Lundstrom & Lindvall, 2023).
Conclusion
The future of AI will undoubtedly be reflected in the practice of diagnostic medical sonography and radiology. It is showing merit in biometry, nodule detection and surveillance, classification of tumours, and image optimization. It is not yet widely integrated with radiology services as the technology still needs refining to be applicable to all hospital and clinic settings and all machine types. This looks like an exciting new future for the world of DI and for patients to experience quicker, more efficient, more standardised imaging with better detection rates.
References
Botwe, B.O., Antwi, W.K., Arkosh, A., et al. (2021). Radiographers’ Perspective on the Emerging Integration on Artificial Intelligence into Diagnostic Imaging: The Ghana Study. Journal of Medical Radiation Sciences, 68(3): 260-268. https://doi.org/10.1002/jmrs.460
Habuza, T., Navaz, A.N., Hashim, F. et al., (2021). AI Applications in Robotics, Diagnostic Image Analysis, and Precision Medicine: Current Limitations, Future Trends, Guidelines on CAD Systems for Medicine. Informatics in Medicine Unlocked, 24. https://doi.org/10.1016/j.imu.2021.100596
Hardy, M. & Harvey, H. (2019). Artificial Intelligence in Diagnostic Imaging: Impact on the Radiography Profession. British Institute of Radiology, 93(1108). https://doi.org/10.1259/bjr.20190840
Kudumala, A., Ressler, D., & Miranda, W. (2020). Scaling up AOI ACross the Life Sciences Value Chain. Deloitte Insight. Retrieved from https://www2.deloitte.com/us/en/insights/industry/life-sciences/ai-and-pharma.html
Liu, S., Wang, Y., Lei B. et al., (2019). Deep Learning in Medical Ultrasound Analysis: A Review. Engineering, 5(2): 261-275. https://doi.org/10.1016/j.eng.2018.11.020
Looney, P., Stevenson, G.N., Nicolaides, K.H. et al. (2018). Fully Automated, Real-time 3D Ultrasound Segmentation to Estimate First Trimester Placental Volume Using Deep Learning. JCI Insight, 3(11). https://doi.org/10.1172/jci.insight.120178
Lundstrom, C. & Lindvall, M. (2023). Mapping the Landscape of Care Providers’ Quality Assurance Approaches for AI in Diagnostic Imaging. Journal of Digital Imaging, 36: 379-387. https://doi.org/10.1007/s10278-022-00731-7
Swar, S., Dent, A., Faust, K. et al. (2019). Physician Perspectives on Integration of Artificial Intelligence into Diagnostic Pathology. NPJ Digital Media, https://doi.org/10.1038%2Fs41746-019-0106-0





Comments