Addressing Healthcare Delivery Challenges in Northern Canada
- Dec 3, 2023
- 9 min read
Updated: Dec 4, 2023

I created this e-portfolio as part of my Master of Health Studies #MHST601 to enhance my online presence and advocate for public health. Initially feeling scattered, I found my passions in digital imaging, patient advocacy, policy streamlining, and travel, particularly in Canada's Northern Territories.
These diverse interests coalesced during the course, guiding me to focus on raising awareness about healthcare challenges in the North. I am committed to promoting culturally appropriate healthcare and equal access, especially for Indigenous populations. To improve healthcare in northern regions, I emphasize understanding geographical, social, economic, and logistical barriers, aligning with the Canadian Health Act (CHA) and Reconciliation Calls to Action. This post will explore strategies to overcome healthcare delivery challenges in the North, address geographical constraints, and discuss social determinants of health, aiming to enhance and modernize the CHA and improve healthcare equality.
Northern Living and Healthcare Delivery Models
Living in Canada's North entails a commitment to a distinctive way of life, with each territory presenting unique landscapes, cultural identities, values, and logistical challenges for its residents. Despite these differences, common limiting factors shape healthcare delivery models across Yukon, Northwest Territories, and Nunavut, characterized by sparse populations spread over vast geographical areas. In Yukon, there are two regional hospitals and one central hospital in Whitehorse offering advanced medical services (Yukon Hospitals, 2023). The Northwest Territories boast four regional hospitals, the largest of which is in Yellowknife (HSSA, 2023), while Nunavut is more limited, relying on air and ice roads for community access, featuring a single hospital in Iqaluit with limited services (Department of Health, 2023). All territories depend on air ambulatory services, subject to weather conditions, compromising timely access to medical services (Yukon Government, 2023; HSSA, 2023; Department of Health, 2023). Due to limited services, many specialists are outsourced to southern provinces, incurring substantial personal and governmental expenses (Clark et al., 2022).

Geography is not the only influencing factor which dictates northern healthcare services. Staff retention is challenging as many report unsustainable working conditions far exceeding their scope of practice, lack of work employment for spouses, isolation, and extreme cost of living. This leads to a constant turnover of healthcare providers, making integration within communities difficult and preventing community members from building trusting and empowering relationships with their healthcare teams (Lee et al., 2020).
Chronic Disease Management and Access to Surgical Services in Canada’s North
Limited medical services in Canada's northern regions communities chronic disease management, as seen in excess osteoarthritis cases needing arthroscopic surgery (ABJHI, 2019; Huot et al., 2019). Sparse populations hinder consistent access to physical and occupational rehabilitation, which is crucial for disease management (ABJHI, 2019; Huot et al., 2019). Understaffed health centers, mainly with nurses and occasional locum physicians, further impede regular access to support and therapeutic healthcare teams necessary for managing osteoarthritis (Lawford & Giles, 2016). More data from territorial governments is needed to ensure accurate assessment of the increased need for arthroscopic surgery in these areas (Statistics Canada, 2019). Given the logistical challenges for surgical services in northern communities, prioritizing robust community-based chronic disease management is vital (Lundstrom & Lindvall, 2023). Failure to provide these services can contradict the CHA’s mandate for, “timely access to medically necessary health services regardless of his or her ability to pay for those services” (CHA, 2015).

Residents in Canada's northern regions need help accessing timely specialist services. One notable example I explored in a previous blog, is that of orthopaedic surgeries, particularly for conditions like knee osteoarthritis (Sakanovic et al., 2022; CIHI, 2023). In Yukon, despite having two full-time orthopaedic surgeons, the current wait time as of 2023 is 18-24 months (Ho, J., 2023). In Nunavut, where orthopaedic services are nonexistent, residents are flown to Ontario, experiencing an average provincial wait time of 14.6 weeks as of 2022. However, this duration likely underestimates the delays for Nunavut residents due to additional logistical challenges in transportation for primary care assessment, diagnostic imaging (only available in Iqaluit), and surgical consultations (Sakanovic et al., 2022). These wait times far exceed the recommended 6-month threshold set by the Alberta Joint and Bone Clinic (ABJB, 2019), leading to prolonged periods of compromised quality of life for patients awaiting diagnostic services and specialist consultations. There are no data collection services for the Northwest Territories, but orthopedic services are offered in Yellowknife (Statistics Canada, 2019).
Future of De-centralized Medicine: Telehealth Services

To bridge the gap caused by centralized health and medical travel, Telemedicine platforms are gaining trust among physicians and patients as they offer valuable solutions in healthcare accessibility (Swar et al., 2019). Emphasizing these strategies can empower patients to manage their health effectively (Lundstrom & Lindvall, 2023; Sakanovic et al., 2023). This approach benefits remote patients or those flown out for medical services by eliminating unnecessary in-person visits
and follow-ups. Particularly impactful in Nunavut, where 18% of the healthcare budget addresses transportation costs to fly-in communities, Telemedicine eases not only financial burdens but also fosters patient-centred care by involving family, elders, and support networks (Lavoie et al., 2023). Additionally, telemedicine optimizes specialist time, reducing wait times for surgical referrals and procedures (Sakanovic et al., 2022). Embracing telemedicine signifies a step towards egalitarian healthcare, aligning with CHA values and socioeconomic principles at various levels. This approach is anticipated to be integral in delivering affordable, accessible, and accountable healthcare in Canada, particularly benefiting remote Northern communities deserving of improved access to services.
Health Factors of Indigenous People in Yukon, Northwest Territories, and Nunavut
In #MHST601, we delved into the social determinants of health (SDoH) and the socioeconomic model (SEM) to address health disparities. SDoH, such as education and financial security, directly impact individual and community health (Leonardi, 2018). SEM expands on these concepts, providing context for how factors beyond a patient's control contribute to unequal health outcomes at various levels: Individual, Interpersonal, Community, Organization, and Policy (White, F.M.M. 2015). Recognising cultural and historical contexts is crucial to understanding their impact on health outcomes and healthcare needs.

Providing culturally sensitive care requires a profound understanding of the demographics, historical influences, and socioeconomic requirements of the people who inhabit the North. Indigenous People constitute substantial proportions of northern populations, reaching up to 86% in Nunavut, 51% in Northwest Territories, and 23% in Yukon (Annual Report to Parliament, 2020). This demographic makeup significantly shapes health definitions, values, historical perspectives, and community needs. Colonial racism and intergenerational trauma have created stark disparities in health determinants and socioeconomic status between Indigenous and non-Indigenous Canadians (Dready, 2019). Providing inclusive health means going beyond standardized health and working towards culturally appropriate and patient-community-centred care.
Health literacy among Indigenous people remains lower than those of non-Indigenous Canadians (Annual Report to Parliament, 2020). Low health literacy correlates with adverse health outcomes, hindering patients in seeking medical care, navigating complex healthcare systems, and complying with healthcare management plans (Palumbo, R. 2016). Addressing health disparities requires supporting programs which address literacy rates among Indigenous People (Nutbeam & Lloyd, 2018). Providing healthcare services in their primary languages, particularly in Nunavut, where 65.3% speak Inuktitut at home, can also support health literacy initiatives (Statistics Canada, 2019). Culturally appropriate healthcare literacy emerges as a paramount concern to enhance access to care and advocate for Indigenous Northern communities, chronically underserved and underfunded.

Because of low literacy rates, Indigenous people experience a median income lower than that of non-Indigenous or off-reserve Indigenous Canadians, frequently placing them in lower socioeconomic brackets (Annual Report to Parliament, 2020). This economic disparity poses a considerable challenge for these individuals in accessing essential services, mainly due to the high transportation burden. Additional costs associated with accessing healthcare, such as gas, mileage, airfare, food, and accommodation, are borne by the patients, often rendering these services financially unfeasible. While all territorial governments have established transportation guidelines, numerous patients still struggle with the financial strain from secondary costs, hindering their right to equitable healthcare access and leading to enduring adverse health outcomes (CHA, 2015). This challenge is evident in the management of chronic diseases, exemplified by osteoarthritis. Access to sustainable and applicable preventive therapeutic practices is crucial for enhancing longevity and delaying surgery. Unfortunately, these services are seldom available locally and typically require patients to bear the associated expenses.
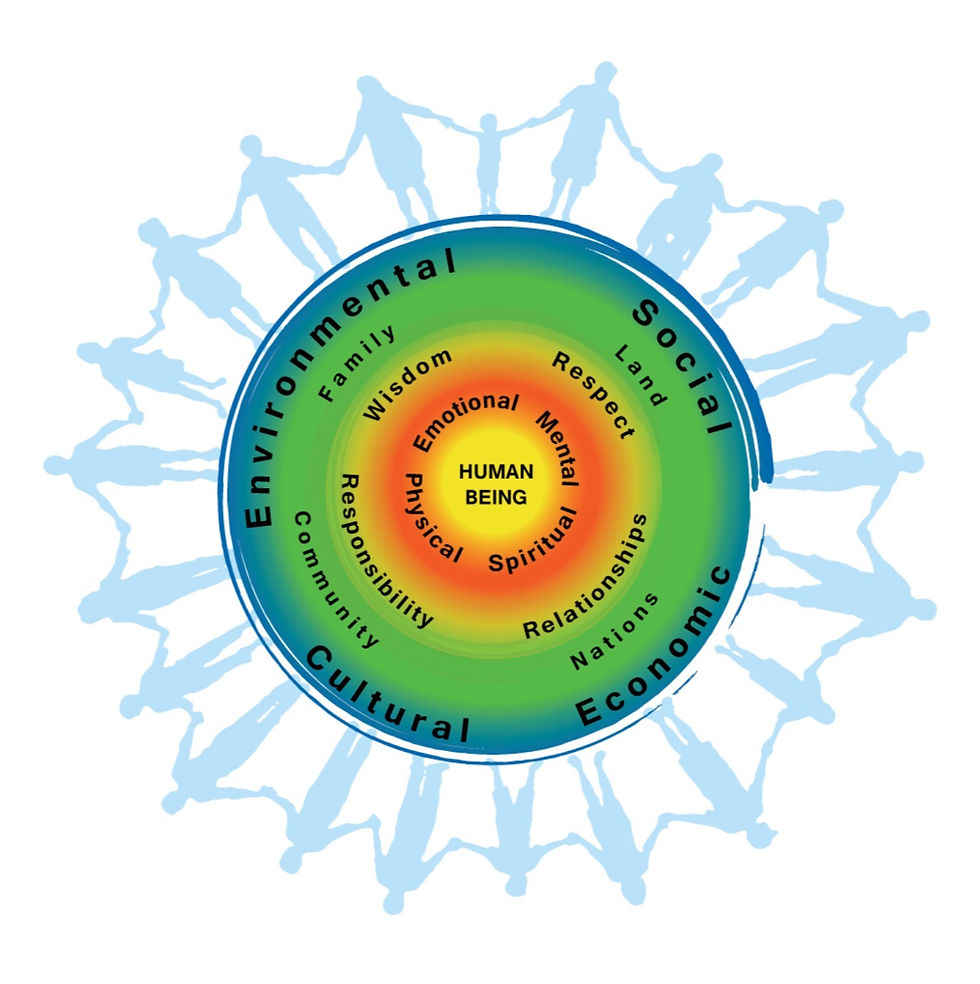
Finally, in many Indigenous cultures, the involvement of healers, elders, and communities is integral to supporting and advocating for sick individuals. However, limited community-based health resources and reliance on external specialist services undermine this approach. Medical evacuations exacerbate challenges for those with low literacy, disconnecting them from their culture and intensifying the vulnerability and isolation experienced during challenging times (Lee et al., 2022). This isolation becomes more evident when considering traditional definitions of physical, mental, spiritual, and community health, where elders and traditional healers play crucial roles in the outcomes of Indigenous patients (Lee et al., 2022).
Future of Northern Healthcare
Living in northern regions profoundly shapes individuals' lives, fostering strong connections to cultural values, health definitions, and the land, especially in large Indigenous communities. To honour this spirit, it is crucial to modernize the CHA and ensure reasonable access to quality care for Northern communities. Addressing staffing shortages is paramount in better supporting community and specialist services. Staff members must undergo cultural competency training, encompassing an understanding of the role of colonization and residential school systems in current health disparities facing Indigenous Canadians (DHSS, 2022). The Truth and Reconciliation Commission of Canada (2015) recognizes the value of Indigenous healing practices and recommends their incorporation in the treatment of Indigenous patients, involving healers and elders to restore a sense of community and cultural identity. Future healthcare models should collaborate with Indigenous governments, fostering territorial solid, federal, and Indigenous governmental relationships to reduce disparities in the North. Additionally, promoting Indigenous healthcare providers fluent in community languages is crucial for effective communication and reducing stigma in healthcare (Lawford & Giles, 2016). Regional healthcare services in Indigenous languages would be a progressive initiative to enhance access and compliance with health management plans.

Conclusion
#MHST601 deepened my appreciation of healthcare challenges in Canada's north. Striving to bolster my online presence and advocate for public health, I've recognized the interplay of geographical, social, economic, and logistical barriers. Disparities in healthcare, notably in chronic disease management like osteoarthritis, highlight the need for strategic actions aligned with the CHA and Reconciliation Calls to Action.

Telemedicine emerges as a promising solution, mitigating the challenges of centralized health systems and medical travel. This shift toward decentralized medicine aligns with the egalitarian principles of the CHA, particularly benefiting remote Northern communities, providing improved access, and empowering patients in health management.
The future of northern healthcare requires modernizing the CHA for reasonable access, particularly for Indigenous communities. Addressing staffing shortages, providing cultural competency training, and incorporating Indigenous healing practices are vital. Understanding unique health perspectives, values, and historical contexts is critical to applying SDoH and SEM principles to
address disparities. Acknowledging colonialism's impact, embracing cultural appropriateness, and promoting individualized, patient/community centered care is essential. Ultimately, the future must prioritize inclusivity, cultural sensitivity, and equitable access in Canada's Northern Territories.
References
Alberta Bone and Joint Health Institute, ABJHI (2019). The Osteoarthritis Crisis in Alberta: Access, Quality, and Long-Term Planning, The AHS Bone and Joint Health Strategic Clinical Network, version 2. https://www.albertaboneandjoint.com/wp-content/uploads/2019/10/ABJHI_Osteoarthritis_Crisis_in_Alberta_2019.pdf
Annual Report to Parliament (2020). Government of Canada. Retrieved from https://www.sac-isc.gc.ca/eng/1602010609492/1602010631711
Buskens, E., Feenstra, T., L., Jorg, F., Kan, K., Lokkerbol, J., Mihalopoulos, C., Schoervers, R. A. (2021). More Than Cost-Effectiveness? Applying a Second-Stage Filter to Improve Policy Decision Making. Health Expectations: An International Journal of Public Participation in Health Care and Health Policy, 24(4), 1413-1433. https://doi.org/10.1111/hex.13277
Canada Health Act, CHA (2015). Annual Report 2014/2015. Retrieved from https://www.canada.ca/content/dam/hc-sc/migration/hc-sc/hcs-sss/alt_formats/pdf/pubs/cha-ics/2015-cha-lcs-ar-ra-eng.pdf
Canadian Institute for Health Information, CIHI (2023). Joint Replacement Wait Times. CIHI. Retrieved from https://yourhealthsystem.cihi.ca/hsp/inbrief#!/indicators/004/joint-replacement-wait-times/;mapC1;mapLevel2;/
Clark, W., Lavoie, J.G., McDonnell et al., (2022). Trends in Inuit Health Services Utilisation in Manitoba: Findings from the Qanuinngitsiarutiksait Study. International Journal of Circumpolar Health, 81(1). doi: 10.1080/22423982.2022.2073069
Department of Health (2023). Medical Travel. Government of Nunavut.. Retrieved from https://www.gov.nu.ca/health/information/medical-travel#:~:text=To%20be%20eligible%20for%20medical,for%20all%20medical%20travel%20costs.
Department of Health and Social Services, DHSS (2022). Family and Children’s Services Annual Report 2020-2022. Yukon Government. Retrieved from https://yukon.ca/sites/yukon.ca/files/hss/cfsa_annual_report_2020-2022.pdf
Flood, C., M. & Thomas, B. (2016). Modernizing the Canadian Health Act. Dalhousie Law Journal, 39(2), 396-411.
Health Canada (2015). Canada Health Act: Annual Report 2014-2015. Government of Canada. Retrieved from https://www.canada.ca/content/dam/hc-sc/migration/hc-sc/hcs-sss/alt_formats/pdf/pubs/cha-ics/2015-cha-lcs-ar-ra-eng.pdf
Health and Social Services Authority, HSSA (2023). Programs and Services. Government of Northwest Territories. Retrieved from https://www.nthssa.ca/en/services
Ho, J. (April 26,2023). Patients Waiting Longer for Joint Replacement Surgeries in Yukon. CBC North. https://www.cbc.ca/news/canada/north/patients-waiting-longer-for-joint-replacement-surgeries-in-yukon-1.6822579
Huot, S., Ho, A., Lam, S. et al. (2019). Identifying Barriers to Heatlhcare Delivery and Access in the Circumpolar North: Important Insights for Health Profesionals. International Journal of Circumpolar Health, 78(1). https://doi.org/10.1080/22423982.2019.1571385
Lavoie, J.G., Clark, W., McDonnell, L. et al (2022). Kivalliq Inuit Women Travelling to Manitoba for Birthing: Findings from the Qanuinngitsiarutiksait Study. BCM Pregnancy and Childbirth, 22:870. https://doi.org/10.1186/s12884-022-05214-9
Lawford, K.M & Giles, A.R. (2016). Kivalliq Inuit Centre Boarding Home and the Provision of Prenatal Education. International Journal of Circumpolar Health, 9(75). doi: 10.3402/ijch.v75.32213
Lee, E., Gudmundson, B., & Lavoie, J.G. (2022). Returning Childbirth to Inuit Communities in the Canadian Arctic. International Journal of Circumpolar Health, 81(1). doi: 10.1080/22423982.2022.2071410
Leonardi, F. (2018). The Definition of Health: Towards New Perspectives. International Journal of Health Services, 48(4), 735–748. https://www.jstor.org/stable/48513032
Lundstrom, C. & Lindvall, M. (2023). Mapping the Landscape of Care Providers’ Quality Assurance Approaches for AI in Diagnostic Imaging. Journal of Digital Imaging, 36: 379-387. https://doi.org/10.1007/s10278-022-00731-7
Nutbeam, D. & Lloyd, J.E. (2021). Understanding and Responding to Health Literacy as a Social
Determinant of Health. Annual Review of Public Health: 42: 159-173. https://doi.org/10.1146/annurev-publhealth-090419-102529
Sakanovic, A., Hadden W.J., Guglani, S. et al., (2022). The Effect of eConsult on the Provision of Orthopaedic Services in Nunavut. International Journal of Circumpolar Health, 81(1). https://doi.org/10.1080%2F22423982.2022.2151551
Senate of Canada (2002). The Health of Canadians – The Federal Role: Chapter Seventeen: The Canadian Health Act, Vol. 6. Standing Committee Social Affairs, Science and Technology. https://sencanada.ca/en/content/sen/committee/372/soci/rep/repoct02vol6part7-e#:~:text=The%20principle%20of%20universality%20of,covered%20by%20provincial%2Fterritorial%20plans.
Statistics Canada (2019). Evolution of the Language Situation in Nunavut, 2001 to 2016. Retrieved from https://www150.statcan.gc.ca/n1/pub/89-657-x/89-657-x2019010-eng.htm
Swar, S., Dent, A., Faust, K. et al. (2019). Physician Perspectives on Integration of Artificial Intelligence into Diagnostic Pathology. NPJ Digital Media, https://doi.org/10.1038%2Fs41746-019-0106-0
World Health Organization. (2019). WHO Strategic Meeting on Social Determinants of Health: Final Meeting Summary. Switzerland. https://cdn.who.int/media/docs/default-source/documents/social-determinants-of-health/14138_legislation_manual_summary_dec17_final.pdf?sfvrsn=d5a289b6_5&download=true
White, F.M.M (2015). Primary Health Care and Public Health: Foundations of Universal Health Systems. Medical Principles and Practice. DOI:10.1159/000370197
Yukon Hospitals (2023). Important Information About Coming to Hospital. Yukon Hospital Corporation. Retrieved https://yukonhospitals.ca/en/about-us/important-information-about-coming-hospital




Comments